What Is Bone Grafting in Dentistry? Complete Guide to Procedure, Types, Cost & Recovery
Losing a tooth affects more than just your smile. When a tooth is gone, the jawbone that once supported it begins to shrink. This process, called bone resorption, happens naturally because the bone no longer receives stimulation from the tooth root. Over time, this bone loss can make it difficult to get dental implants or lead to changes in your facial structure.
Bone grafting offers a proven solution. This dental procedure rebuilds lost or weakened jawbone, creating a strong foundation for implants and helping preserve your natural facial contours. Whether you’ve lost teeth due to injury, gum disease, or extraction, bone grafting can restore what’s been lost and open the door to effective tooth replacement.
This guide explains everything you need to know about dental bone grafting—from understanding why it’s needed to what happens during the procedure, how long recovery takes, and what it costs in India.
What Is Bone Grafting in Dentistry?
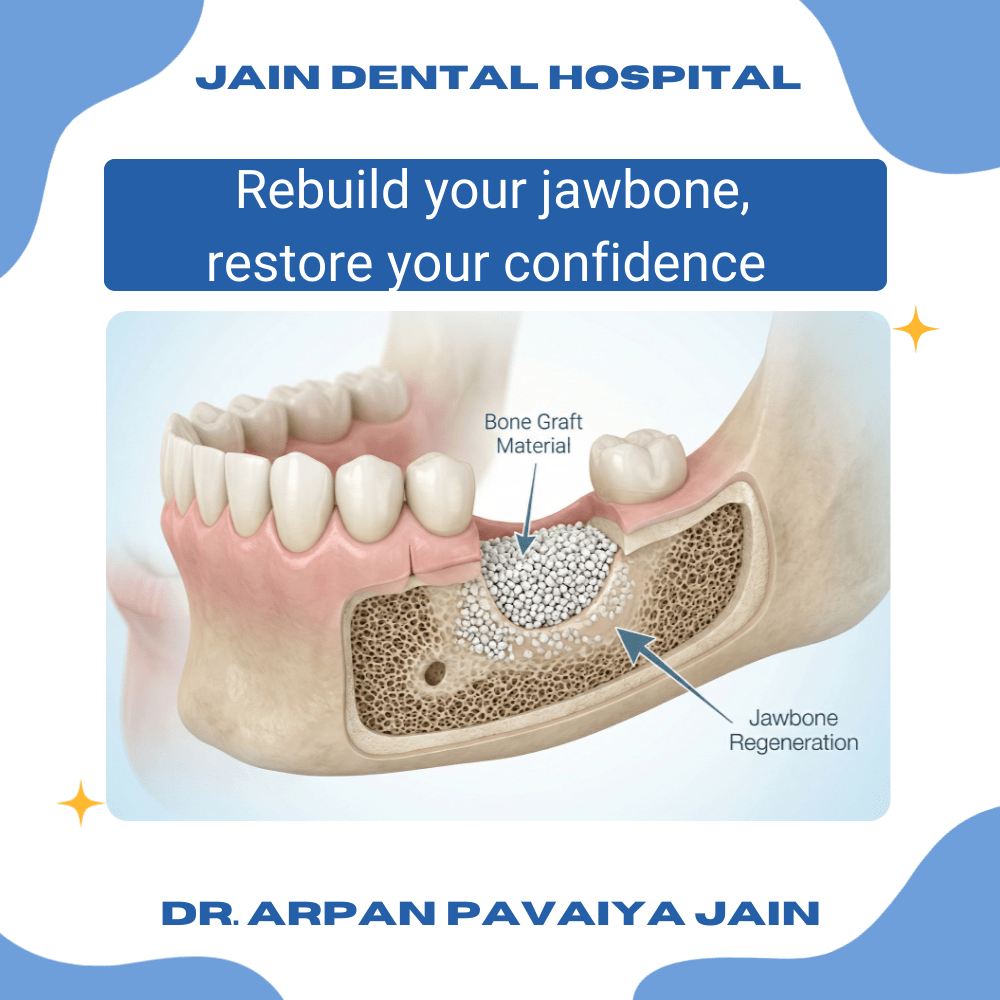
Bone grafting is a surgical procedure that adds bone or bone-like material to areas of your jaw where bone has been lost or weakened. Think of it as building a scaffold that encourages your body to grow new, healthy bone in that spot.
The grafting material can come from different sources—your own body, a donor, an animal source, or a lab-made synthetic. Once placed in the jaw, this material acts as a framework. Over the following months, your natural bone cells grow into and around the graft, eventually replacing it with strong, living bone.
Dentists and oral surgeons perform bone grafting procedures regularly. According to clinical research, More than 2.2 million bone graft procedures are performed worldwide each year across medical and dental fields. The procedure has become a standard part of modern dentistry, especially for patients preparing for dental implants.
Why Is Bone Grafting Needed?
Bone grafting becomes necessary when the jawbone lacks the density or volume required to support dental treatments or maintain oral health. Several factors can lead to bone loss in the jaw.
Tooth Loss and Bone Resorption
When you lose a tooth, the bone that once anchored it starts to deteriorate. Without the pressure and stimulation from chewing, your body redirects calcium from that area to other parts of your skeleton. This process can begin within weeks of tooth loss and continues progressively.
The longer a tooth remains missing, the more bone is lost. This makes future dental implant placement difficult or even impossible without first rebuilding the bone through grafting.
H3 Gum Disease (Periodontitis)
Advanced gum disease doesn’t just affect your gums—it destroys the bone supporting your teeth. Bacterial infection causes inflammation that breaks down bone tissue over time. As the bone deteriorates, teeth become loose and may eventually fall out.
Bone grafting can help restore lost bone structure and stabilize remaining teeth. It also prepares the area for implants if teeth have already been lost to periodontal disease.
Trauma or Injury
Accidents, sports injuries, or facial trauma can damage or fracture the jawbone. Even grinding your teeth (bruxism) puts excessive pressure on your jaw, which may contribute to bone and tooth support problems.
Bone grafts can repair these damaged areas, restoring both function and structure to your jaw.
Preparation for Dental Implants
Dental implants require adequate bone to hold the titanium post securely. If you don’t have enough bone density or volume, the implant may fail. This is where bone grafting becomes essential—it creates the strong foundation needed for successful implant placement.
A significant proportion of implant cases require bone grafting to ensure long-term success.
Types of Bone Grafts Used in Dentistry
Different grafting materials serve different purposes, and your dentist will choose the best option based on your specific needs.
Autograft (Your Own Bone)
An autograft uses bone taken from another part of your body—typically from your chin, jaw, or hip. Because it’s your own tissue, your body accepts it readily, and it contains living cells that promote bone growth.
Benefits: Autografts are considered the gold standard because they offer the highest success rates and fastest healing. There’s no risk of rejection since the bone comes from your own body.
Considerations: The main drawback is that it requires a second surgical site to harvest the bone, which can lead to additional discomfort and a longer recovery period.
Allograft (Donor Bone)
Allografts use bone tissue from a human donor, typically obtained from a tissue bank. The bone is thoroughly processed, sterilized, and treated to remove all cells that could trigger an immune response.
Benefits: No second surgical site is needed, which means less discomfort and a shorter procedure. Allografts are widely available and have good success rates.
Considerations: While extensively tested for safety, some patients prefer not to use donor tissue. Healing may take slightly longer compared to autografts.
Xenograft (Animal-Derived Bone)
Xenografts come from animal sources—most commonly cows (bovine) or pigs (porcine). The organic components are removed, leaving only the mineral structure that supports new bone growth.
Benefits: Xenografts are readily available, cost-effective, and eliminate the need for a second surgical site. They provide a stable scaffold for your natural bone to grow into.
Considerations: Some patients have ethical or religious concerns about using animal-derived materials. The integration process can take longer than with autografts.
Alloplast (Synthetic Bone Material)
Alloplasts are man-made materials designed to mimic natural bone. Common examples include hydroxyapatite (a naturally occurring mineral found in bones), calcium phosphate, and bioactive glass.
Benefits: These materials are completely synthetic, avoiding any concerns about donor tissue or animal products. They’re readily available and can be manufactured to specific specifications.
Considerations: Synthetic materials may not integrate as quickly as natural bone, and long-term success rates can vary depending on the specific material used.
Types of Bone Grafting Procedures
Not all bone grafts are the same. The type of procedure you need depends on where the bone loss occurred and what you’re preparing for. Here are the most common bone grafting procedures performed in dentistry.
Socket Preservation
Socket preservation is the most common type of bone graft, typically performed immediately after a tooth extraction. When a tooth is removed, the empty socket begins to collapse and lose bone volume within weeks.
How it works: Your dentist fills the empty socket with grafting material right after extraction. This preserves the bone’s shape and volume, making it ready for an implant later.
Timeline: The graft typically heals in three to six months, after which an implant can be placed.
When it’s used: Socket preservation is ideal for patients who plan to get dental implants in the future but aren’t ready for immediate placement.
Ridge Augmentation
Ridge augmentation rebuilds the width and height of the jawbone when significant bone loss has occurred. This procedure is necessary when the jaw has become too narrow or shallow to support implants.
How it works: The dentist places bone grafting material along the ridge (top edge) of your jaw where teeth once stood. Sometimes, a protective membrane is placed over the graft to guide bone regeneration.
Timeline: Healing takes four to six months before implants can be placed.
When it’s used: Ridge augmentation is common for patients who have been missing teeth for an extended period or who have experienced severe bone loss due to gum disease.
Sinus Lift (Sinus Augmentation)
A sinus lift is a specialized procedure for the upper jaw, specifically in the area of the premolars and molars. The maxillary sinuses (air-filled spaces in your skull) sit just above the upper back teeth. When teeth are lost in this area, the sinuses can expand downward, leaving insufficient bone for implants.
How it works: Your oral surgeon lifts the sinus membrane upward and places bone grafting material in the space created underneath. This increases the bone height needed to support implants.
Timeline: Sinus lifts typically require six to nine months of healing before implant placement.
When it’s used: This procedure is necessary when there’s less than 5–6 millimeters of bone height in the upper back jaw.
Periodontal Bone Grafting
Periodontal bone grafting treats bone loss caused by gum disease. Unlike other grafts that prepare for implants, this procedure aims to regenerate bone around existing teeth to stabilize them.
How it works: The dentist cleans out infection and diseased tissue, then places grafting material in the areas where bone has been destroyed by periodontitis.
Timeline: Initial healing takes a few weeks, but full bone regeneration can take several months.
When it’s used: This procedure helps save teeth that have become loose due to bone loss from gum disease.
Step-by-Step Bone Grafting Procedure
Understanding what happens during the procedure can help ease any anxiety you might feel. Here’s what you can expect from start to finish.
Consultation and Imaging
Your journey begins with a thorough examination. Your dentist will review your medical history, discuss your symptoms, and take X-rays or a 3D CBCT scan to assess your bone density and determine exactly where grafting is needed.
This imaging helps your dentist plan the procedure precisely, choosing the right type and amount of grafting material for your specific situation.
Local Anesthesia
On the day of your procedure, your dentist will numb the treatment area with local anesthesia. You’ll feel pressure during the procedure but no pain. If you’re particularly anxious, sedation options are available to help you relax.
Placement of Graft Material
Once the area is numb, your dentist makes a small incision in your gum tissue to expose the underlying bone. The grafting material is then carefully placed in the area where bone is needed.
The amount of material used depends on the extent of bone loss. For minor defects, only a small amount is needed. For larger defects, more substantial grafting is required.
Membrane Placement (If Required)
In many cases, your dentist will cover the graft with a thin protective membrane. This barrier keeps the graft material in place and guides bone regeneration by preventing soft tissue from growing into the area too quickly.
Some membranes dissolve naturally as you heal. Others need to be removed during a follow-up visit.
Suturing and Healing Phase
After the graft and membrane are in place, your dentist repositions the gum tissue and closes the incision with stitches. These sutures typically dissolve on their own within one to two weeks.
The entire procedure usually takes 45 minutes to two hours, depending on the complexity and number of sites being grafted.
How Long Does Bone Grafting Take to Heal?
Healing from a bone graft happens in stages, and patience is essential for successful results.
Initial Recovery (1–2 Weeks)
The first week after surgery involves soft tissue healing. You may experience mild to moderate swelling, bruising, and discomfort during this time. These symptoms are normal and should gradually improve.
Your gums will start to heal over the graft site, and any stitches will dissolve or be removed during a follow-up appointment.
Bone Integration Phase (3–6 Months)
This is when the real work happens. Your natural bone cells gradually grow into and around the graft material, replacing it with living bone. Most dental bone grafts need at least three months to heal, though complete healing can take up to one year for larger grafts.
During this phase, you won’t notice much happening externally, but inside your jaw, new bone is forming and strengthening.
Ready for Implant Placement
Once your bone graft has fully integrated—typically after four to six months—your dentist will take another X-ray to confirm adequate bone growth. If everything looks good, you can proceed with dental implant placement.
It’s important to note that if you wait too long after your graft has healed (beyond 6–12 months), the new bone can begin to resorb if not stimulated by an implant. Your dentist will advise you on the optimal timing for your implant procedure.
Is Bone Grafting Painful?
One of the most common concerns patients have is about pain. The good news is that bone grafting is generally well-tolerated and causes minimal discomfort.
During the Procedure
You won’t feel pain during the surgery because the area is completely numbed with local anesthesia. If you’re anxious, sedation dentistry options can help you feel more relaxed throughout the procedure.
After the Procedure
Once the anesthesia wears off, you may experience some tenderness, swelling, and mild pain. Most patients describe the discomfort as similar to what you’d feel after a tooth extraction—manageable with over-the-counter pain relievers or prescribed medication.
Applying ice packs to your face for the first 24–48 hours helps reduce swelling and discomfort. The pain typically peaks within the first two to three days and gradually subsides over the following week.
Pain Management Tips
- Take pain medication as prescribed or recommended by your dentist.
- Use ice packs on your face (20 minutes on, 20 minutes off) for the first two days.
- Keep your head elevated, especially when sleeping.
- Avoid touching or disturbing the surgical site.
- Stick to soft foods and avoid chewing on the grafted area
Most patients report that the procedure is much less uncomfortable than they anticipated.
Risks and Complications
Bone grafting is a safe, routine procedure, but like any surgery, it carries some potential risks. Being aware of these helps you recognize any problems early and seek prompt treatment.
Swelling and Minor Bleeding
Mild swelling and some bleeding are normal in the first few days after surgery. However, if swelling worsens after the first week or if bleeding doesn’t stop with gentle pressure, contact your dentist.
Infection Risk
Infection is rare but possible. Signs include persistent pain that gets worse instead of better, fever above 101°F (38.3°C), pus or discharge from the surgical site, and a foul taste or smell in your mouth.
Your dentist will prescribe antibiotics to reduce infection risk. Taking them exactly as directed is essential.
Graft Failure (Rare)
In rare cases, the graft may fail to integrate with your natural bone. This can happen if:
- The graft becomes exposed through the gum tissue
- Infection develops
- You smoke (nicotine restricts blood flow and impairs healing)
- You have uncontrolled diabetes or other health conditions that affect healing
Signs of graft failure include persistent pain or swelling after the first week, gum recession around the graft site, and no improvement in bone volume on follow-up X-rays.
If graft failure occurs, your dentist will discuss options, which may include repeating the procedure after allowing the area to heal.
Nerve Damage
Though extremely rare, there’s a small risk of nerve damage during the procedure, particularly for grafts in the lower jaw. This could result in temporary or, very rarely, permanent numbness in the lip, tongue, or chin.
Your oral surgeon takes great care to avoid nerves during the procedure. If you experience any unusual numbness that doesn’t improve within a few weeks, inform your dentist immediately.
Cost of Bone Grafting in India
The cost of bone grafting varies significantly based on several factors. Understanding these can help you plan and budget for the procedure.
Average Price Range
Based on data from dental clinics across India, here are typical cost ranges for different bone grafting procedures:
Socket Preservation: ₹15,000 – ₹25,000
This procedure is performed immediately after tooth extraction to preserve bone for a future implant.
Single Tooth Bone Grafting: ₹2,000 – ₹8,000
For minor bone loss around a single tooth site.
Ridge Augmentation: ₹25,000 – ₹45,000
This more extensive procedure rebuilds significant bone loss along the jaw ridge.
Indirect Sinus Lift: ₹8,000 – ₹12,000
A less invasive sinus augmentation procedure.
Direct Sinus Lift: ₹15,000 – ₹25,000
A more complex sinus lift requiring surgical access from the side of the jaw.
Block Bone Graft: ₹40,000 – ₹60,000
For severe bone loss requiring a larger bone block graft.
Factors Affecting Cost
Several variables influence the final price of your bone grafting procedure:
Type of Graft Material: Autografts tend to be more expensive because they require harvesting bone from another site. Synthetic materials and xenografts are generally less costly.
Complexity and Extent: Larger grafts or multiple sites being treated will increase the cost.
Geographic Location: Dental treatment costs vary by city. Metropolitan areas like Mumbai, Delhi, and Bangalore typically have higher prices than smaller cities.
Clinic and Surgeon Expertise: Experienced oral surgeons and well-equipped clinics may charge more, but this often translates to better outcomes and fewer complications.
Additional Procedures: If you need CT scans, advanced imaging, or membrane placement, these add to the total cost.
Does Insurance Cover Bone Grafting?
Most dental insurance plans in India don’t cover dental implants, but coverage for bone grafting varies. Some plans may cover bone grafts if they’re medically necessary—for example, if the graft treats bone loss from periodontal disease or trauma.
However, if the graft is performed solely to prepare for cosmetic dental implants, it’s less likely to be covered. Check with your insurance provider to understand your specific coverage before proceeding.
Success Rate of Dental Bone Grafting
Bone grafting has high success rates when performed by experienced surgeons and when patients follow proper aftercare instructions.
According to Clinical studies report very high success rates (often above 90–95%), and some specific cohorts have shown 100% graft success over several years of follow‑up, depending on the type of graft and individual patient factors. Research published in systematic reviews shows that:
- Block bone grafts achieve success rates of 95–100% with survival rates of 97–100%.
- Implants placed in grafted sites have success rates ranging from 84–97% after follow-up periods of up to 10 years.
- These rates are comparable to implants placed in natural, ungrafted bone.
Factors That Improve Success
Several factors contribute to successful bone graft outcomes:
Experienced Surgeon: Choose a qualified oral surgeon or periodontist with extensive bone grafting experience.
Quality Graft Material: High-quality grafting materials promote better integration and faster healing.
Patient Health: Good overall health, controlled blood sugar (if diabetic), and a strong immune system support healing.
Non-Smoking: Smoking significantly reduces success rates by restricting blood flow to the healing site.
Proper Aftercare: Following your dentist’s post-operative instructions carefully is critical for success.
Aftercare Tips for Faster Healing
Proper aftercare makes a significant difference in how quickly and successfully your bone graft heals. Here’s what you need to do.
Foods to Eat and Avoid
For the first few days after surgery, stick to soft foods that require minimal chewing:
Good choices include:
- Yogurt and smoothies
- Mashed potatoes
- Scrambled eggs
- Soup (lukewarm, not hot)
- Oatmeal
- Protein shakes
- Soft pasta
Avoid:
- Hard or crunchy foods (chips, nuts, raw vegetables)
- Sticky or chewy foods (caramel, gum)
- Very hot foods or beverages
- Spicy foods that may irritate the surgical site
- Alcohol (for at least two weeks)
Gradually reintroduce normal foods as healing progresses, but avoid chewing directly on the grafted area until your dentist gives you the green light.
Oral Hygiene Instructions
Keeping your mouth clean is essential to prevent infection, but you must be gentle around the surgical site.
For the first 24 hours:
- Don’t rinse your mouth vigorously
- Avoid brushing near the surgical site
- Don’t spit forcefully (let saliva drip into the sink instead)
After 24 hours:
- Gently rinse with warm salt water (1/2 teaspoon salt in 8 ounces of water) two to three times daily
- Carefully brush your teeth, avoiding the grafted area
- After a few days, you can gently brush around the surgical site with a soft-bristled toothbrush
Avoid:
- Using straws (the suction can dislodge the graft)
- Smoking or vaping
- Vigorous swishing or spitting
Activity Restrictions
Rest is important for healing. Here’s what to avoid:
- Strenuous exercise or heavy lifting for at least 48 hours (ideally one week)
- Bending over or activities that increase blood pressure in your head
- Blowing your nose forcefully (especially if you had a sinus lift)
- Light walking is fine and actually promotes healthy circulation.
Follow-Up Visits
Attend all scheduled follow-up appointments. Your dentist needs to monitor healing progress, remove any non-dissolving sutures, and address any concerns before they become problems.
If you experience any of the following, contact your dentist immediately:
- Fever above 101°F (38.3°C)
- Severe pain that doesn’t improve with medication
- Heavy bleeding that doesn’t stop with gentle pressure
- Signs of infection (pus, foul odor, increased swelling)
Frequently Asked Questions (FAQ)
Can bone grow back naturally?
Once bone is lost in the jaw due to tooth loss or disease, it doesn’t regenerate on its own. The body requires stimulation from tooth roots to maintain bone density. Without intervention through bone grafting, lost bone will not return naturally.
How do I know if I need a bone graft?
Your dentist will determine if you need a bone graft through clinical examination and imaging studies like X-rays or CT scans. Common indicators include tooth loss, visible bone loss on X-rays, loose teeth due to gum disease, or insufficient bone for dental implant placement.
Can smokers undergo bone grafting?
Yes, but smoking significantly reduces success rates. Nicotine restricts blood flow, which impairs healing and bone integration. Most oral surgeons strongly recommend quitting smoking at least two weeks before surgery and throughout the healing period for the best results.
Is bone grafting necessary before implants?
Not always. If you have adequate bone density and volume naturally, you can proceed directly to implant placement. However, many patients—especially those who have been missing teeth for some time—require bone grafting to create a strong foundation for successful implant integration.
What happens if I don’t get a bone graft?
Without adequate bone, dental implants may fail or cannot be placed at all. Additionally, continued bone loss can lead to changes in facial structure, a sunken appearance, difficulty wearing dentures, and potential problems with remaining teeth.
Conclusion: Make Bone Grafting Work for Your Smile
Bone grafting is a proven, reliable procedure that rebuilds lost jawbone and creates the foundation necessary for successful dental implants. While the healing process requires patience—typically three to six months—the results are worth the wait.
With very high success rates in many studies and well-established techniques, bone grafting has become a routine part of modern dentistry. If you’re facing bone loss due to missing teeth, gum disease, or trauma, don’t wait. The sooner you address bone loss, the better your options for restoration.
Schedule a consultation with an experienced oral surgeon or periodontist to discuss your specific situation. With proper diagnosis, skilled treatment, and diligent aftercare, you can restore your jawbone, protect your oral health, and move forward with confidence toward a complete, functional smile.
Schedule Your Consultation Today
Rebuild the Foundation for a Strong, Lasting Smile — With Expert Care
Now that you understand what bone grafting is, why it’s needed, and how it supports successful dental implants, the next step is determining whether your jawbone is ready for treatment. Not every case of bone loss is the same, and the right grafting approach depends on your bone volume, implant goals, and overall oral health.
At Jain Dental Hospital, Dr. Arpan Pavaiya Jain and Dr. Rashi Agarwal Jain carefully evaluate your jawbone using advanced imaging such as CBCT scans to assess bone density and plan precise grafting procedures. Whether you require socket preservation, ridge augmentation, or a sinus lift before implant placement, we focus on predictable healing, long-term implant stability, and patient comfort.
If you’ve been told you may not have enough bone for implants — or you’re unsure about your eligibility — a professional evaluation can provide clarity and a structured treatment plan tailored to your needs.
📞 Call: +91-9582535204
🌐 Visit: www.jaindentistdelhi.com

Dr. Arpan Pavaiya Jain, Director of Jain Dental Hospital, Indirapuram, Ghaziabad is a renowned Prosthodontist and Implantologist with over 20 years of expertise in advanced dentistry. A graduate of the prestigious King George’s Medical College Lucknow, he has performed more than 20,000 successful dental implant procedures. Dr. Jain leads a team of skilled professionals, offering state-of-the-art treatments in dental implants, clear aligners, cosmetic dentistry, orthodontics, and more. Known for his personalized care and commitment to excellence, he has earned a reputation as a trusted dental expert in Indirapuram, Ghaziabad.